- 5 Simple Tips For Breastfeeding A Small Baby - February 5, 2026
- Supporting Immigrant Families Through Birth: 5 Organizations To Support - January 29, 2026
- Podcast: How Emotional Support Can Change Lives In Childbirth with Founder Suzzie Vehrs - January 23, 2026
🤔 Midwife vs. OB-GYN: Who’s Your Pregnancy Pal? 🤰
Hello, dear readers! 🌟 Whether you’re embarking on the exciting journey of pregnancy for the first time or adding a new member to your growing family, understanding your options for prenatal care is essential. 🤰👶
In this blog post, we’re going to dive into the wonderful world of pregnancy care and explore the differences between two remarkable healthcare professionals: the trusty midwife 🌼 and the renowned OB-GYN 👩⚕️👨⚕️. It’s time to break down the stereotypes, unravel the mysteries, and make your care provider decision not just a bit more informed but also a tad more fun! 🎉
So, let’s get ready to embark on this enlightening adventure, and demystify the roles of midwives and OB-GYNs in your pregnancy story. 🌟💕
Why Might It Matter If You Pick A Midwife Vs OB GYN For Your Pregnancy Care And Birth?

Choosing between a midwife and an OB-GYN is like selecting your pregnancy BFF, and it’s a decision that can profoundly impact your journey. Why does it matter? Well, here’s the lowdown:
While both midwives and OB-GYNs share the overarching goal of ensuring a healthy mom and baby, they bring unique philosophies, purposes, and knowledge to the table. 🌟
Midwives are experts in normal pregnancies and excel at addressing the holistic needs of expectant mothers. What happens when our physical and emotional needs get met? We flourish.
A recent study linked midwifery care from hospital-based midwives to 30% to 40% lower rates of C-section for low-risk women.
In addition, women in midwifery care have been shown to have fewer interventions, fewer c-sections, fewer preterm babies, and fewer severe tears and complications in general. All at a lower cost.
On the flip side, OB-GYNs are superheroes when it comes to complex medical scenarios. They were trained in pathology – which is the study of disease. Because of this, they specialize in helping pregnant mothers with recognized diseases or serious complications. They excel at ensuring the safest outcome for both mothers and little ones, especially when a pregnancy has left the space of low-risk. 🏥
So, the choice between a midwife and an OB-GYN ultimately depends on your preferences and unique circumstances. It’s an adventure designed just for you. 😉🌟👶 Let’s delve deeper into each role.
Midwife vs. OB-GYN: Decision Making

One of the fundamentals of the midwifery model of care is joint decision making. In the midwifery model, it is believed that pregnancy and childbirth involve every part of you. Your feelings, hopes, fears, physical and practical needs, and spiritual or religious beliefs can all affect your pregnancy and birth. A midwife providing the Midwifery Model of Care addresses all of these aspects to help you give birth naturally, safely and confidently.
On the other hand, in the OB-GYN model of care, you’ll often encounter a more structured expert-novice relationship. Here, the physician typically assumes primary responsibility for decisions, often due to legal and hospital regulations. This can result in a more directive approach, where you might receive specific instructions rather than engaging in collaborative decision-making. ⚖️🏥
Midwife vs. OB-GYN: Birth Locations

You may be surprised to learn that midwives often deliver babies at hospitals. They can also attend births at independent birth centers or even home births. Typically, if you work with a midwife at a hospital, you will have a CNM – this is a Certified Nurse Midwife. A CNM has an advanced nursing degree with a doctorate in Midwifery.
If you give birth at an independent birth center or home birth, you are most likely working with a CPM – this is a Certified Professional Midwife. A CPM usually holds a master’s degree in midwifery and attended hundreds of births during her training. However the path to licensure varies from state to state.
OB GYNs only deliver babies at the hospital. Of course, they attended medical school. In this time they gained a few skills above and beyond what a midwife learns. OB GYNS can do vacuum or forcep assisted deliveries and perform a c-section. Neither of which you will see a midwife doing.
Midwife vs. OB-GYN: Prenatal Visits

What’s in store for your prenatal visit with a midwife or OB-GYN? 🤰👩⚕️
While both have the same mission – keeping you and your bun-in-the-oven healthy – the way they roll out the prenatal red carpet can be quite different.
You can expect that you will have a physical examination, fetal monitoring, medication review, and appropriate tests done with both a Midwife and an OB. Let’s take a peek behind the curtain and see how they do these same things differently! 🎬👀
Midwife Magic: ✨ Midwives believe in quality time! You can expect visits lasting 30 minutes to a full hour. 🕐 They’re all about the partnership, making sure you’re actively involved in your care. Ultimately, you are the decision maker, and it’s important that they provide you with enough information and space for you to make a aligned choices about your birth. 🤝🌟
OB-GYN Express: 🏥 Now, the medical model is all about efficiency. OB-GYNs are pros at spotting issues, so if you don’t have a problem, it’s assumed you’re A-okay. Visits with them are usually quick, lasting 10 to 15 minutes. 🕒💨 If there’s an issue, they’re like speedy superheroes with prescription pads. They’re all about fixing what needs fixing. 🦸♀️💊
So, whether it’s a laid-back chat with your midwife or a lightning-fast check-in with your OB-GYN, the goal is the same: a healthy and happy pregnancy journey! 🤗👶❤️
Let’s Give An Example Of The Difference
Let’s dive into the world prenatal appointments deeper by comparing experiences of morning sickness – a rite of passage for many expecting moms! 🤢🤰
With my second daughter, Hazel, under the watchful eye of my midwife, things played out a bit like this: When the nausea hit, my midwife and I embarked on a nutritional quest. We chatted about what I was eating, she dished out some fantastic natural nausea-busting tips, and we pondered if it was disrupting my daily grind. Then, she peeked at the prenatal vitamin label to check a few choice ingredients. And yep, she even offered a prescription as a backup plan. But you know what? I never had to go down that route – the natural tricks did the job! 🌿🥗🥤
Now, rewind to my first pregnancy with Zoe, and my chat with the OB-GYN took a different spin. When I dared to ask about my diet’s role in my morning sickness, they flashed a reassuring smile and whisked out a prescription for anti-nausea meds. “No worries,” they said, “swing by 7-11 for a Coke Slurpee on your way home, and grab this while you’re out.” Then handed me the prescription.💁♀️💊🥤
So, when you’re pondering between an OB and a Midwife, think about how you like to tackle bumps in the pregnancy road. Are you the natural remedies and look for root causes first type, or do you revel in the quick fixes? There’s no right or wrong here; it’s all about your style. Your choice could be as unique as your pregnancy journey! 🤷♀️👩⚕️💖
Midwife vs. OB-GYN: Pain Management

Pain management is a key player when deciding between a Midwife and an OB-GYN for your pregnancy journey.
In the United States, roughly 60% of expectant mothers opt for the trusty epidural, a pain relief superstar available exclusively in hospitals. Naturally, this often draws those who prefer epidurals towards OB-GYNs for their birth team. 🏥💆♀️
But here’s a curveball: Certified Nurse Midwives (CNMs), known for their versatility in hospital settings, can also offer the epidural experience if that’s your go-to choice. 🌟💉This may be the sweet spot for those that are unsure if they want a natural experience or an epidural experience before labor starts. Or for those that generally prefer holistic care – but definitely want an epidural on the big day.
Now, let’s shift gears to Certified Professional Midwives (CPMs). Typically, they aren’t found in hospitals, so the epidural isn’t part of their playbook. Instead, they’re masters of creating a soothing atmosphere, employing gentle movements, therapeutic touch, hot and cold packs, may suggest a tens unit, and are the experts at the art of mindful breathing. 🌊🧘♀️🌡️ You may also want a doula to help with these things inside or outside of the hospital.
CPMs have witnessed many women bravely embrace natural childbirth and firmly believe in your strength. While their primary goal is to support a natural birthing process, they may offer alternatives like nitrous oxide or other pain management tools if your labor journey takes unexpected twists and turns. 🦸♀️💪
Midwife vs. OB-GYN: Monitoring You And Baby In Labor

Can how you and your baby are monitored during labor impact the chances of a surgical birth? 🤔🏥
Absolutely! When you’re at the hospital with an OB-GYN or a Certified Nurse Midwife, the standard procedure is continuous electronic fetal monitoring. 📊👶 Initially, it might seem like keeping a constant eye on the baby is the safest route, but that’s not always the case. 🚫🚶♀️
Here’s the deal: Continuous monitoring can be a bit tricky when the mama-to-be is on the move. 🚶♀️💃 . And guess what? Movement can actually help the labor process! You may be surprised to find out that continuous fetal monitoring has a false positive rate of 99%. Meaning most of the times it says something is wrong – it’s all good. This also makes it really hard to differentiate the 1% when it’s not.
Research shows that constant fetal monitoring is linked to a higher rate of C-sections, more assisted vaginal births, and maternal infections, without a significant reduction in cerebral palsy or neonatal death when compared to intermittent auscultation (IA). 📈🔍
Another hiccup with electronic fetal monitoring is that it might mean less face time with your care providers. 🙅♀️👨⚕️👩⚕️ While it may seem convenient for them to keep an eye on things from afar, it can lead to decisions being made based on incomplete information. 🤷♀️💼 It also means less support and encouragement for a mama in labor.
Now, let’s talk about who should use what: Women with high-risk conditions like preeclampsia, type 1 diabetes, preterm birth, or suspected intrauterine fetal growth restriction should roll with electronic fetal monitoring (EFM). But if you’re a healthy mama without complications, you might consider intermittent auscultation (IA) also known as Intermittent Monitoring. 🩺👩⚕️
What Is Intermittent Monitoring?
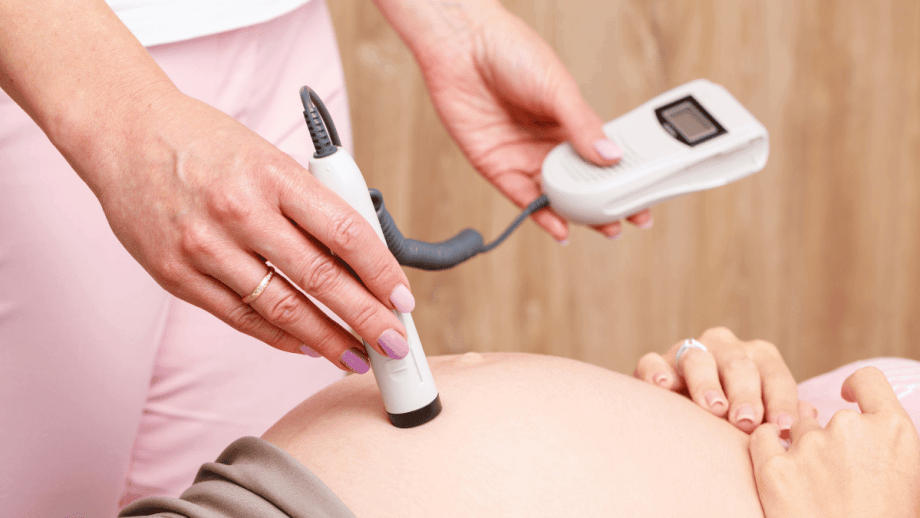
So, what’s intermittent monitoring all about? It’s the go-to method for Certified Professional Midwives (CPMs). They use a nifty handheld doppler to listen to the baby regularly, giving a crystal-clear picture without keeping you glued to one spot. 🎵👣
And here’s the cherry on top: Intermittent monitoring of your baby brings a human touch into the mix, fostering a stronger connection between you and your care provider. 🤗👩⚕️ You end up with extra support and encouragement during your incredible journey through labor and delivery! 🌟👶💪
While this is the go to monitoring method for CPMs in an out of hospital setting, you may be able to request it in a hospital setting. However, I often see this request turned down. Not all hospitals have the training, policies or staff to make intermittent monitoring possible to every mom that walks through their doors. In this case, it’s about resources. Hospitals have invested heavily in machines leaving less room to invest in the manpower (or should I say nurse power💪) needed to fuel intermittent monitoring.
Midwife vs. OB-GYN: Time With You In Labor

Let’s dive into a question that might catch you by surprise: How much time will your OB-GYN, Certified Nurse Midwife (CNM), or Certified Professional Midwife (CPM) spend with you during labor? 🤔🏥
Now, picture this: I’m wearing my doula hat, right there with a laboring mama giving birth at a hospital. We usually make our entrance when contractions are a reliable 5 minutes apart, lasting a solid minute, and have kept up this rhythm for a whole hour. (P.S. You can check out our contractions timing guide here!) ⏱️🤰
So, what’s the scoop once we’re at the hospital? An OB-GYN or CNM typically checks in with us for around 15 minutes initially. Then, they pop back in every 3 to 4 hours for another 10-15 minute check. When it’s go-time, like when a mom is pushing and after delivery when she may need a stitch or two, the OB GYN or CNM is typically around for an hour to 90 minutes. So, if a mom’s labor adventure spans 15 hours after checking into the hospital, the OB-GYN or CNM spends roughly one to two hours in total with her. 🕒👩⚕️
How Does This Compare To An Out Of Hospital Birth?

Now, switch back to me wearing my doula hat, but this time we’re in for an out-of-hospital birth. We wait a little longer to call in the midwife, usually heading to a birth center when contractions are a trusty 3 minutes apart, lasting a minute, and have kept up this groove for an hour. But here’s where it gets interesting: Once the midwife is on the scene, she and her trusty assistant stick around pretty much non-stop until after the birth. 🚀🏡
All in all, a CPM at an out-of-hospital birth spends a solid 5-10 hours supporting a mom on her journey through an average birth. 🌟🤱💪 They spend MUCH more time with each patient. Only attend one patient at a time and naturally build a closer, more encouraging relationship with their patients because of this.
If you are wondering what YOU as can do to support labor either in the hospital or at home to manage contractions, move through each stage and work effectively with your care provider, make sure to join our birth course right away. We’ll get you equipped with the tools you need!
Midwife vs. OB-GYN: Emergencies

Emergencies – those unexpected twists in the childbirth journey that keep us on our toes. But how do OB-GYNs compare to CNMs or CPMs in handling these high-stress moments? 🚑🏥
Here’s the scoop: When it comes to emergencies, OB-GYNs are the seasoned superheroes. If you’re at the hospital and your birthing path veers from low risk to high risk, the OB-GYN team swoops in to save the day. The on-duty doctor steps in to navigate through the unexpected hurdles. This might involve using forceps or a vacuum to assist with a tricky delivery, or in some cases, performing surgery to safely bring your baby into the world. 🦸♂️✂️👶
The good news? Hospitals always have OB-GYNs on call, so if you started with a CNM, the transition of care is usually seamless. And if you were already under the care of an OB-GYN, well, they’ve got you covered from start to finish. 🤝🏨
Now, what if your precious little one needs some extra TLC after they make their grand entrance? Don’t worry – the hospital has a squad of skilled nurses ready to lend a helping hand. They can swiftly clear those tiny lungs, offer necessary medication, or provide oxygen if your baby needs it. 🌬️👶💙
Of course, nobody wants to imagine their baby facing challenges right from the get-go, but it’s reassuring to know that help is right there if it’s ever needed. 💪👩⚕️👨⚕️
How Are Emergencies Handled At Out Of Hospital Births?

Certified Professional Midwives usually only work with low risk mamas. Most of the time, a birth with a CPM is uncomplicated. But – that doesn’t mean they aren’t ready for emergencies.
If your birth isn’t progressing, you decide you need an epidural, or your baby seems to have an okay, but not great heart rate, indicating something could go wrong later, a CPM will have to transfer a mother from her care into the care of an OB GYN at the hospital.
Yup, you heard right. You get not only a provider change, but a location change. Typically, this means you and your partner drive carefully to the hospital and you are met at the door with a wheelchair. However, if the situation is truly emergent, you would go in an ambulance.
On the other hand, you may be surprised how many tools a Certified Professional Midwife has with her. It’s almost like she brings the hospital to your home.
What Is In A CPMs Go Bag?
Tools Used At Every Birth:
In a CPM’s trusty bag, you’ll find a bunch of essentials used in every birth:
🩸 Blood draw supplies
🔊 Fetal Doppler (the MVP for listening to baby’s heart tones during prenatal checkups and labor)
🩺 Blood pressure cuff
🌡️ Thermometer
👶 Newborn scale
👂 Adult and newborn stethoscopes
🩺 A glucometer
🚽 Urine dipsticks
…and maybe a few other handy tools that come in clutch! 🧰🤓 These items are used at every single birth to make sure a mama and baby duo are well monitored and watched over throughout labor.
Emergency Medications For Moms
When it comes to birth emergency medications, a CPM at a home birth or birth center is fully equipped with the essentials, all legally obtained and administered. They are also some of the most common medications used in the hospital. Here’s the lowdown: 💊🏠
- Pitocin: The go-to superhero medication for tackling postpartum hemorrhage. Administered through intramuscular injection or IV, it’s like a wake-up call for the uterus, causing powerful contractions that help stop the bleeding. 💪🩸
- Methergine: Another trusty sidekick in the battle against postpartum hemorrhage. This one enters the scene through an intramuscular injection, focusing its energy on those lower uterine contractions to save the day. 🦸♀️🌊
- Misoprostol: A third hero in pill form, swooping in to assist with postpartum hemorrhage by triggering those life-saving uterine contractions. 💊🩸
- Tranexamic Acid: The fourth and final member of the hemorrhage-fighting squad. This one has a unique strategy—it stops bleeding by encouraging blood clotting, putting an end to the flow. 🩸🚫
- Terbutaline: Reserved for super rare emergencies, this ace is called upon to halt uterine contractions when necessary. 🚨❌
- Herbs: Nature’s allies! 🌿 Cotton Root Bark and Black Cohosh join forces to stem bleeding by giving the uterus a gentle nudge. And let’s not forget about Yunnan Baiyao, the Chinese herb that’s all about boosting blood clotting. 🌱🩸
- Syringes and Alcohol Pads: These sidekicks are always at the ready to assist in delivering the above medications, making sure everything goes smoothly. 💉🧼
Rest assured, when it comes to a home birth with a midwife, preparedness is the name of the game, and safety is the top priority! 🏡👩⚕️🌟
Emergency Materials For Baby
Safety is paramount, and this includes having the necessary equipment and expertise to ensure the baby’s well-being. 🏡👶🌟
One crucial set of tools that significantly enhances home birth safety is the newborn resuscitation supplies, along with the essential skills and training to use them effectively when required. These supplies include:
- An ambu bag, which is used to assist a baby’s breathing.
- A resuscitation board equipped with a warmer to maintain the baby’s temperature, suction equipment to clear airways, an oxygen tank, and a newborn mask.
- A newborn pulse oximeter to assess the baby’s oxygen levels.
While most babies make a smooth transition into the world without any need for intervention, a small percentage may require extra assistance to begin their journey. With these tools and comprehensive training in newborn resuscitation, the midwife can swiftly and confidently provide intervention when necessary, ensuring the baby’s well-being without delay. 🌟👩⚕️👶
A Midwife Brings Herself
Indeed, the ultimate key to ensuring safety during a home birth is the experienced and skilled midwife herself. With a wealth of experience in managing emergencies and a sharp sense of discernment, a proficient midwife is the most vital resource in the birthing journey. 🏡👩⚕️🌟
While the majority of births unfold smoothly without the need for medications or an abundance of equipment, having these tools readily available, just in case, offers an extra layer of reassurance and security for both the mother and the midwife. 🩺🔧🤗
Midwife vs. OB-GYN: PostPartum

Let’s delve into one last important aspect when comparing a Midwife to an OB-GYN – the post-baby care. After giving birth at a hospital, whether with a CNM or an OB-GYN, you’ll typically stay there for observation spanning 24 to 48 hours. During your stay, you’ll have access to a team of professionals, including lactation specialists, nurses, baby doctors, and specialists who will be in and out of your room constantly and provide support and care as needed. 🏥👩⚕️👶
Now, let’s talk about the postpartum checkups. In the past, these were often limited to a single visit scheduled 4 to 6 weeks after giving birth. However, ensuring comprehensive care for a new mom’s health in just a 30-minute visit can be quite challenging. 🗓️💼
That’s where the American College of Obstetricians and Gynecologists (ACOG) steps in. They recommend that new moms maintain regular contact with their ob-gyns throughout the 12 weeks following childbirth. The first checkup should occur within the initial 3 weeks post-birth, ensuring that mothers receive the continuous care and attention they need during this crucial period. 👩⚕️🤝🌟
Though this is more than what was previously given, I still wish more support was provided. Especially by lactation counselors, physical floor PTs and therapists that are more equipped to handle the specific physical and emotional challenges of postpartum – which are not typical diseases and therefore out of the scope of care of most OB GYN and only loosely included in the more holistic scope of CPMs.
What Is Care After Birth Like With A CPM?

Following a birth at a birth center or in the comfort of your home, a dedicated midwife will typically keep a close watch over you during the crucial hours after childbirth. 🏡👩⚕️👶
Once you’ve been discharged from the birth center, their caring team, whether it’s a birth center nurse or midwife, will schedule a home visit at approximately 24 hours postpartum to ensure everything is going smoothly. They’ll then return for another home visit at around the 3-day mark after giving birth. 🗓️🏠👁️
These initial postpartum home visits are typically followed by scheduled office visits, usually occurring at 10 days to 2 weeks after birth and again at 4 to 6 weeks postpartum. Additionally, they’ll provide follow-up support via phone and offer additional in-person visits as needed to ensure your continued well-being during this transformative time. ☎️🏥💖
Again, CPMs offer more time and a holistic approach in this sensitive time. But also consider lactation counselors, pelvic floor PTs and therapists as part of your full post partum care team.
PS You may also like our guide to Postpartum Recovery and Perineal Tear Recovery: Healing Stitches Quicker After Birth.
TL/DR Summary: 🤔 Midwife vs. OB-GYN: Who’s Your Pregnancy Pal? 🤰

When it comes to selecting your pregnancy care provider, the wonderful thing is that you have choices! 😃 This means your personality, values, approach, and birth plan should all play a role in your decision-making. While there may be significant distinctions between OB-GYNs and midwives, they both come with their own unique strengths. Furthermore, every provider is an individual with their own set of values and experiences.
It’s worth noting that some OB-GYNs truly embrace the midwifery model of care, just as some midwives may not always take the slow and collaborative approach. Additionally, you can research the c-section rates at your local hospitals to find one that has a proven track record of providing excellent care to mothers and babies in your area. 🏥🔍
So, consider your specific needs and preferences, and don’t hesitate to meet with multiple providers before making the final decision that’s right for you. Your pregnancy journey should align with your values and expectations! And you deserve not great, but excellent care. 😊👶🌟🤰



